SOAP notes are the backbone of veterinary medical documentation. A well-written SOAP note protects you legally, ensures continuity of care, and communicates patient status clearly. But writing detailed SOAP notes takes time—time you could spend with patients.
This guide covers SOAP note structure, provides veterinary-specific templates, and explores how AI tools are transforming documentation in modern practices.
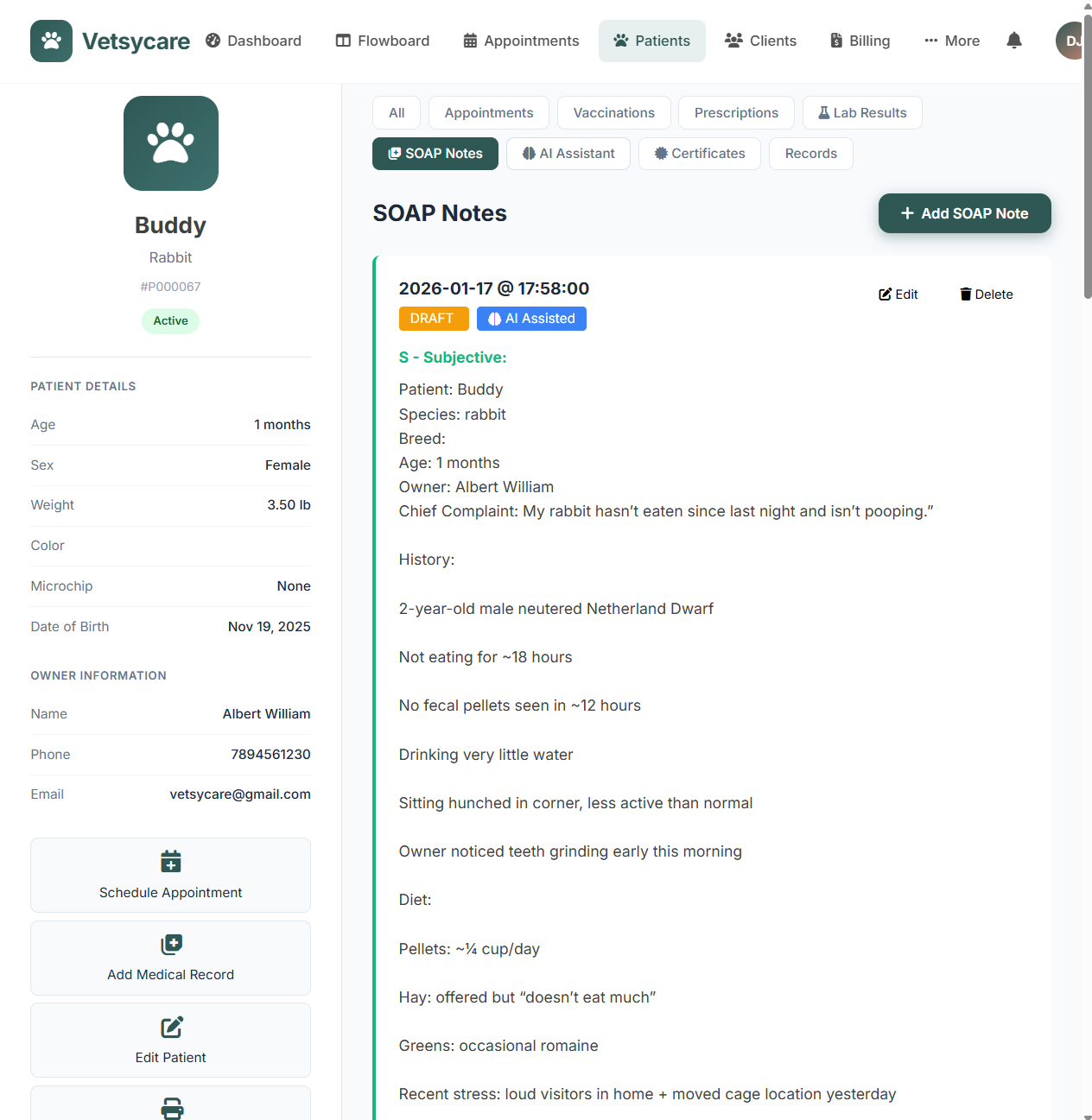
What is a SOAP Note?
SOAP is an acronym for the four sections of a structured medical note:
- S - Subjective: What the owner reports; patient history
- O - Objective: What you observe and measure; physical exam findings, vitals
- A - Assessment: Your diagnosis or differential diagnoses
- P - Plan: Treatment, medications, follow-up, client instructions
This format creates consistent, comprehensive documentation that any veterinary professional can quickly understand.
Why SOAP Notes Matter
Medical-Legal Protection
Thorough documentation is your best defense in case of complaints or litigation. If it wasn't documented, it didn't happen.
Continuity of Care
When another veterinarian sees your patient (emergency, referral, or you're on vacation), good SOAP notes let them pick up seamlessly.
Communication
SOAP format creates a shared language across your team—everyone knows where to find specific information.
Quality Improvement
Reviewing past SOAP notes helps identify patterns, evaluate treatment outcomes, and improve your clinical decisions.
SOAP Note Structure in Detail
S - Subjective
Record information from the pet owner and patient history:
- Chief complaint: Why is the pet here today?
- History of present illness: Duration, progression, associated symptoms
- Owner observations: Changes in behavior, appetite, elimination
- Current medications: What the pet is currently taking
- Allergies: Known drug or food reactions
"Owner reports Max has been vomiting for 3 days, 2-3 times daily, usually after eating. Decreased appetite since yesterday. Normal drinking. No diarrhea noted. Last bowel movement this morning, appeared normal. No known toxin exposure. No recent diet changes. Current on heartworm prevention (Heartgard). No known allergies."
O - Objective
Document your findings from physical examination and diagnostics:
- Vital signs: Temperature, heart rate, respiratory rate, weight
- General appearance: Mentation, body condition, hydration
- Systems examination: Findings organized by body system
- Diagnostic results: Lab work, imaging, other test results
"T: 101.8°F, HR: 110 bpm, RR: 24/min, Weight: 28.4 kg (down from 29.1 kg at last visit)
General: QAR, BCS 5/9, mild dehydration (skin tenting ~2 sec)
EENT: Clear ocular discharge, ears clean, oral exam normal
Cardiovascular: Regular rhythm, no murmur, pulses strong and synchronous
Respiratory: Clear lung sounds, no increased effort
Abdominal: Mild discomfort on palpation of cranial abdomen, no masses palpated, bladder small
Lymph nodes: WNL
Musculoskeletal: Ambulatory x4, no lameness
CBC/Chem: Pending"
A - Assessment
Document your clinical thinking:
- Primary diagnosis: Your most likely explanation
- Differential diagnoses: Other conditions to consider, ranked by likelihood
- Problem list: All active issues identified
- Clinical reasoning: Why you're thinking what you're thinking
"Acute gastritis/gastroenteritis - most likely given history and mild abdominal discomfort
Differential diagnoses:
1. Dietary indiscretion
2. Foreign body - less likely given normal appetite until recently, but cannot rule out
3. Pancreatitis - mild presentation possible
4. Metabolic disease - less likely in young dog, will evaluate with bloodwork"
P - Plan
Document your treatment plan clearly:
- Diagnostics ordered: Tests and imaging
- Treatments administered: In-clinic procedures
- Prescriptions: Medications with dosing
- Client instructions: Home care, diet, activity restrictions
- Follow-up: When to return, what to watch for
- Prognosis: Expected outcome
"Diagnostics: CBC, chemistry panel, abdominal radiographs
Treatments: SQ fluids 300ml LRS administered; Cerenia 1mg/kg SQ administered
Prescriptions:
• Cerenia (Maropitant) 24mg tablet - Give 1 tablet by mouth once daily for 4 days
• Famotidine 10mg - Give 1 tablet by mouth twice daily for 7 days
Client instructions: Bland diet (boiled chicken and rice) in small frequent meals for 3-5 days. Withhold regular food for 12 hours, then introduce bland diet. Ensure fresh water available. Monitor for continued vomiting, lethargy, bloody stool, or lack of appetite.
Follow-up: Recheck in 3-5 days if not improving. Call immediately if vomiting worsens, bloody vomit, severe lethargy, or complete anorexia.
Prognosis: Good with symptomatic treatment if uncomplicated gastroenteritis."
Veterinary SOAP Note Templates
Use these templates as starting points. Customize based on your practice preferences.
General Wellness Exam Template
S: Presenting for wellness exam. Owner reports [no concerns / concerns with...] Appetite: [normal/increased/decreased] Drinking: [normal/increased/decreased] Energy: [normal/increased/decreased] Elimination: [normal/abnormal - describe] Current medications: [list or none] Current diet: [brand/type, amount, frequency] O: T: ___°F HR: ___ bpm RR: ___/min Weight: ___ kg General: [mentation, BCS, hydration] EENT: [eyes, ears, nose, throat] Oral: [teeth, gums, tartar grade] CV: [rhythm, murmur Y/N, pulses] Resp: [lung sounds, effort] Abd: [palpation findings] LN: [palpable nodes] MS: [gait, joints] Integument: [skin, coat] Neuro: [if assessed] A: [Age]-year-old [breed] [intact/neutered] [male/female] - Overall health status - Any issues identified P: Vaccines: [list administered] Parasite prevention: [recommendations] Dental: [grade, recommendations] Recommendations: [list] Next visit: [timeframe]
Sick Patient Template
S: Presenting for [chief complaint] Duration: [how long] Progression: [getting better/worse/same] Frequency: [if applicable] Associated signs: [other symptoms observed] Changes in: appetite/drinking/urination/defecation/activity Current medications: [list] Allergies: [list or NKDA] Recent events: [boarding, diet change, toxin exposure, etc.] O: T: ___°F HR: ___ bpm RR: ___/min Weight: ___ kg General: [mentation, BCS, hydration status] [Focused exam findings based on complaint] Diagnostics: [Results or "pending"] A: Problem list: 1. [Primary problem] - [differential diagnoses] 2. [Secondary problem if applicable] P: Diagnostics: [ordered tests] Treatments administered: [list] Prescriptions: - [Drug, dose, frequency, duration] Client instructions: [home care] Monitoring: [what to watch for] Follow-up: [when, under what circumstances] Prognosis: [expected outcome]
How AI is Changing SOAP Note Documentation
Artificial intelligence is revolutionizing veterinary documentation in several ways:
Voice Dictation with Auto-Structuring
Modern AI dictation goes beyond simple speech-to-text:
- Speak naturally during your exam—no special commands or formatting
- AI recognizes context and sorts content into S, O, A, P sections
- Veterinary vocabulary accuracy (drug names, conditions, anatomical terms)
- Edit and approve rather than write from scratch
Time savings: Veterinarians using AI dictation report saving 30-45 minutes per day on documentation.
Template Auto-Population
AI can pull relevant information from patient history to pre-fill templates:
- Previous diagnoses and ongoing issues
- Current medications
- Last vital signs for comparison
- Vaccination status
Diagnostic Suggestions
Some AI systems analyze your Subjective and Objective findings to suggest:
- Differential diagnoses ranked by likelihood
- Recommended diagnostics based on presentation
- Standard treatment protocols
SOAP Note Best Practices
Be Specific
- ❌ "Abdomen normal"
- ✅ "Abdomen soft, non-painful on palpation, no masses or organomegaly appreciated"
Document Negatives
Recording what you didn't find is just as important as what you did:
- "No murmur auscultated"
- "No lameness observed"
- "No masses palpated"
Use Objective Language
- ❌ "Dog seemed uncomfortable"
- ✅ "Dog exhibited guarding behavior and vocalized on abdominal palpation"
Time-Stamp Important Events
For hospitalized patients or procedures, note when things happen:
- "10:45 - Vomited x1, small amount bile"
- "14:30 - Administered Cerenia 1mg/kg SQ"
Complete Every Section
Even if brief, every section should have content. Use "Not assessed" rather than leaving blank if a system wasn't examined.
Common SOAP Note Mistakes
- Incomplete subjective: Missing duration, progression, or relevant history
- Vague objective: "WNL" without specifying what was examined
- Assessment without reasoning: Diagnosis listed but not supported by findings
- Missing client instructions: Plan says "send home meds" without specific guidance
- No follow-up plan: When should the patient return? What signs warrant emergency visit?
- Delayed documentation: Writing notes hours later from memory increases errors
Efficient SOAP Note Workflow
Maximize documentation efficiency:
- Pre-populate before entering room: Pull history, last vitals, ongoing problems
- Document subjective during intake: Technician captures owner report
- Use templates: Don't start from blank page every time
- Dictate during exam: Voice-to-text while examining (with AI structuring)
- Complete before leaving room: Don't let notes pile up
- Review and sign immediately: Fresh memory catches errors
Write SOAP Notes Faster with VetSyCare AI
VetSyCare includes AI-powered voice dictation that automatically structures your notes into SOAP format, plus diagnostic suggestions and drug interaction checking—saving you 30+ minutes daily.
Try VetSyCare FreeFrequently Asked Questions
How detailed should SOAP notes be?
Detailed enough that another veterinarian could understand the case and continue care. When in doubt, err on the side of more detail. Key findings, clinical reasoning, and patient instructions should always be thorough.
Can I use abbreviations?
Standard veterinary abbreviations (WNL, QAR, BCS, etc.) are acceptable. Avoid obscure or practice-specific abbreviations that others might not understand. When in doubt, write it out.
What if I need to correct a SOAP note later?
Never delete or overwrite original documentation. Add an addendum with the current date/time noting the correction and what is being changed. Most PIMS systems handle this automatically with audit trails.
How long should I keep SOAP notes?
Medical record retention requirements vary by state, but typically 5-7 years minimum. Many practices keep records indefinitely since digital storage is inexpensive.